Podcast: Play in new window | Download
Subscribe: Apple Podcasts | Spotify | Android | Pandora | iHeartRadio | TuneIn | RSS
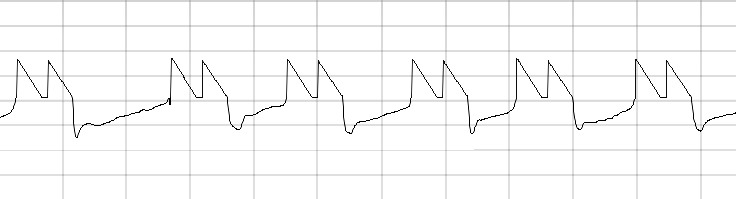
A restless patient experiences a series of dyssynchrony events during mechanical ventilation. Come see how Bryan wades through it all, and allow us to offer an academic, yet practical approach to this sometimes-confusing subject.
Case files

Takeaway lessons
- Start with ABCs and stabilizing the patient, then put on your thinking cap and try to optimize synchrony. It’ll reduce sedation requirements, lessen the risk of lung injury, and prevent mechanical ventilation from feeling like black magic.
- Sedation is a last resort, but sometimes needed if the patient wants something (e.g. more volume) that we think is unwise.
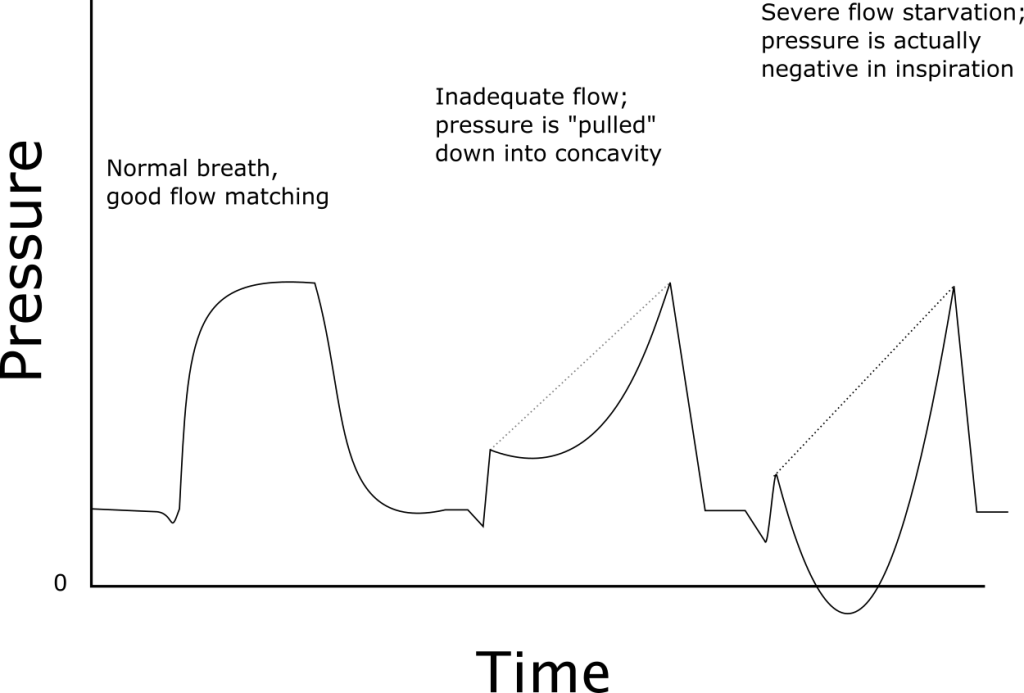
- Most dyssynchrony is the patient fighting the ventilator, so it can often be managed by allowing the patient to determine more variables within the breath. Go from volume control to pressure control, or pressure control to pressure support.
- Sometimes, you won’t figure it out.
- In the decompensating patient, use DOPES to remember the causes
- D isplaced tube
- O bstructed tube
- P neumothorax
- E quipment failure
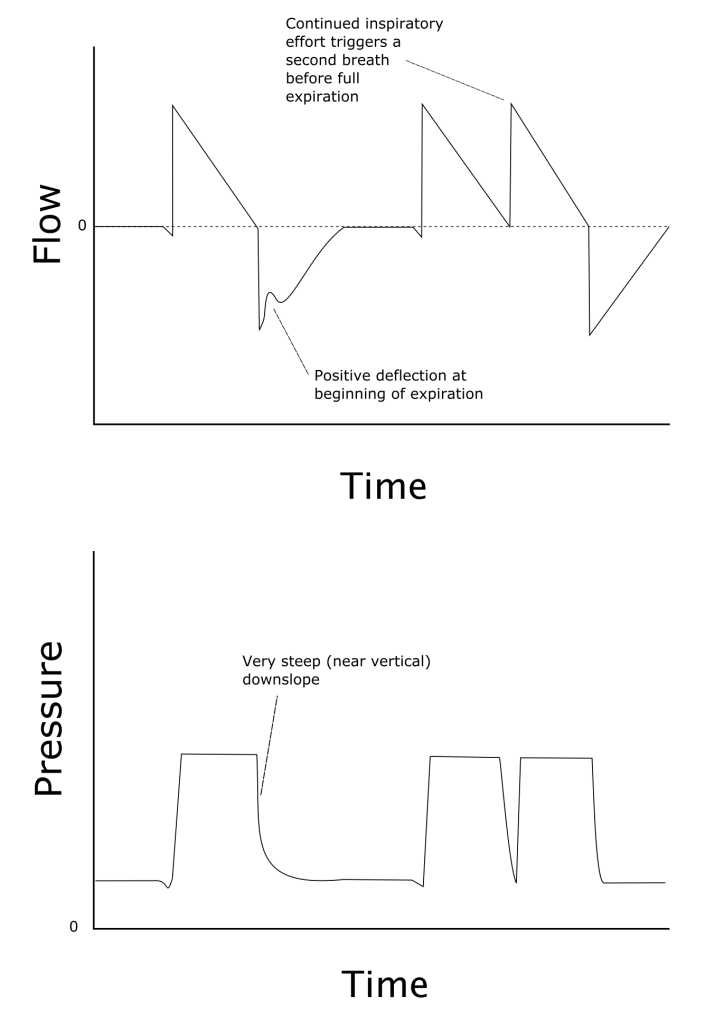
- S tacking of breaths
- Remember “peak pressure apnea,” a phenomenon of iatrogenic hypoventilation caused by the high pressure alarm setting.
Resources
References
- Oto B. Peak pressure apnea: An under-recognized, high-risk form of ventilator asynchrony [published online ahead of print, 2020 Feb 10]. Heart Lung. 2020;S0147-9563(20)30012-1. doi:10.1016/j.hrtlng.2020.01.012

thank you. great podcasts
regarding checking for ETT displacement, before pulling the tube, we can also take a quick look at the vocal cord area with video laryngoscope to see if the balloon of ETT us above the vocal cords. i find this safer then just pulling the tube blindly. Thoughts?